 But typically, we need to have others who know how to properly test the autoclave.” Ultimately, we decided to pare it back and just keep 2 people involved who learned a standardized method. “In other words, they were carrying out the spore testing differently, testing at different times of the day, or placing the test strips in different parts of the unit. They had 4 people conducting spore testing, and they were getting failed test ,” Harvey says. “I recall working with one practice that was struggling with standardization. Having a backup plan is important, because they faced with, ‘How do we go back and identify the instruments that have already been used on patients?’ Unless pouches and cassettes are properly labeled and dated, it can create confusion when trying to identify which instruments need to be resterilized.”īest Practices Although staffing redundancy in the sterilization center is an old idea, too many people can be counterproductive. “They’ll have a traditional, typical-sized autoclave, and then have what’s called a STATIM, which holds a smaller capacity. “Sometimes offices have multiple units,” Harvey observes. Redundancy steps and having a second sterilizer can help in the event of a failed test result. You don’t have to throw out your autoclave if it failed, but you do not want to use it again until you get a negative spore test. A lot of times it fails because of user error. If you get another failed test, you should probably research a little more, maybe call someone to fix it. Ideally you have another autoclave you can use, but you take the failed autoclave out of commission and retest it. “You have to take it back and reprocess it. “You’re supposed to take back everything from the last negative test, because you’ve labeled everything,” Dr Kane says. Worst Case Scenario What should you do in the event of a failed spore test result? The answer, although inconvenient, is designed to minimize infection risk. It’s wise to be familiar with your dental practice act.” However, it’s important to know what the spore testing requirements are in your state or province. Whereas with third-party testing, you may have to wait a week to get the results back.  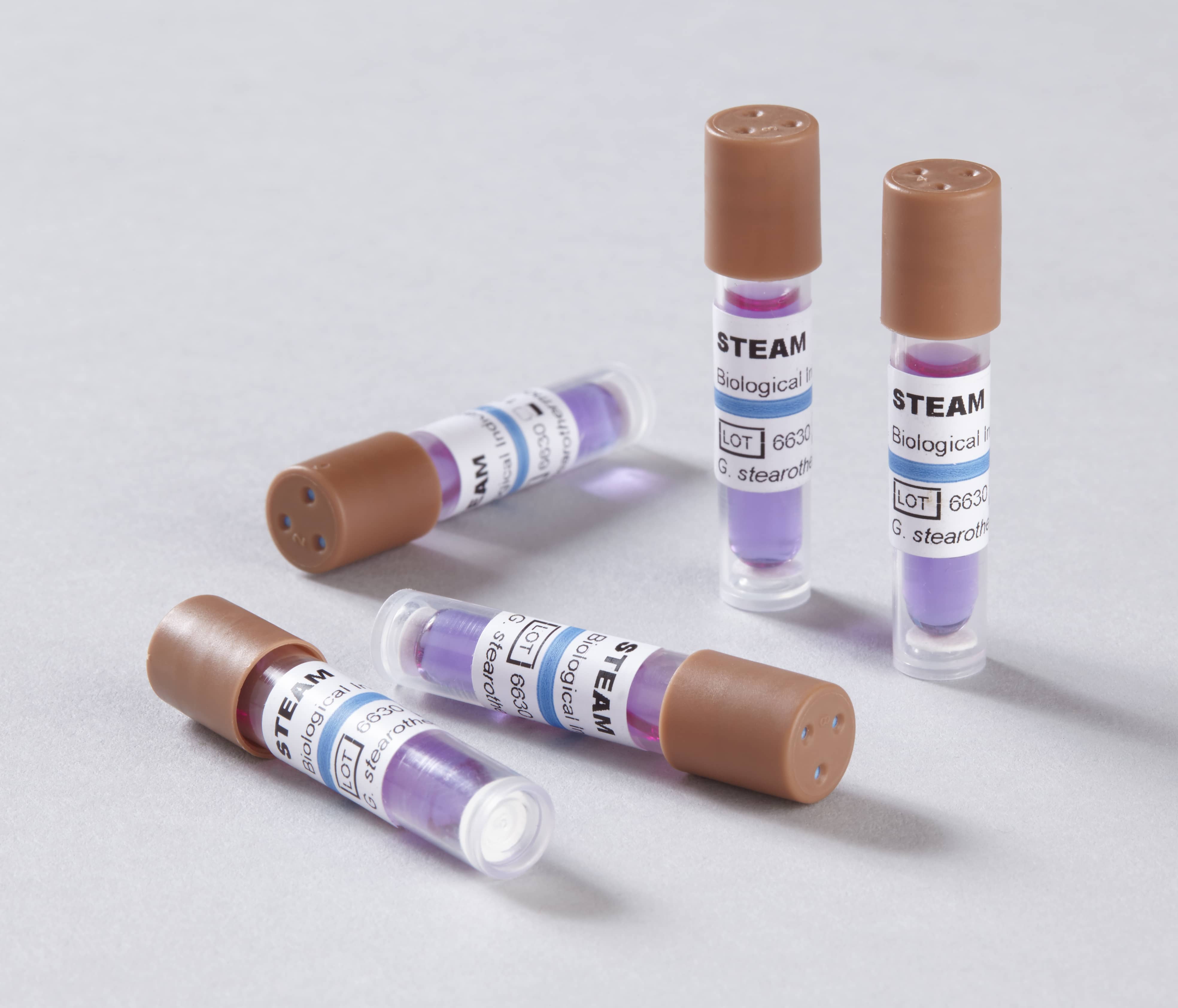
What’s exciting about this new technology is when you can have spore test results in 24 minutes, enables you to immediately begin troubleshooting if you have a failed test. “That way, whether someone leaves the practice, on vacation, or out sick, it’s done. If multiple team members will be conducting the spore testing, the tests must be standardized and ensure everyone is following the exact same process,”Harvey says. “Someone or several team members should be assigned the task of weekly testing. In addition, practices must perform testing on a regular basis, at least weekly. And now there are rapid readout biological indicator tests, and you can get the results in 24 minutes in the office.” “The technology is evolving everywhere in dentistry, not just with ‘dentistry in a day,’ artificial intelligence, or teledentistry. “The technology has changed in this arena,” Harvey says. Double-check with your state and make sure they’re OK with in-office tests.”įortunately, the tests seem to be getting better and better. “There are different options,” Dr Kane observes. Test Types Different types of tests exist with the goal of making the sterilization process faster and more efficient. 
Maintaining the efficacy of your sterilization units is done through weekly spore testing, which assures the instruments are indeed sterilized and able to be safely used on patients.” “All the patient care systems are spokes of that hub, that heart-the sterilization center. “You have to keep that heart pumping well,” Harvey observes. Harvey is the president and founder of The Linda Harvey Group, a health care compliance and risk management consulting company. Harvey, MS, RDH, LHRM, DFASHRM, likens the practice’s sterilization center to the heart of the practice. You have to do a spore test, otherwise you don’t know whether it’s working.” You have to test for biological indicators. And the only way to tell whether your machine is working and doing what it’s supposed to be doing is if you test it. Dr Kane is the owner of Dental Office Compliance of New England LLC and an infection control consultant.“In order for instruments to be clean enough to be in someone’s mouth, they have to be sterilized. “Because you want to know whether the sterilizer works,” Lisa Kane, DMD, says. The necessity for testing should go without saying. But like household dishwashers and washing machines, sterilizers need to be cleaned-and their cleanliness needs to be tested. Because its job is cleaning, it is taken for granted that it exists in a state of eternal cleanliness. Too often the practice’s sterilizer is seen as a household dishwasher or washing machine. 
0 Comments
Leave a Reply. |
AuthorWrite something about yourself. No need to be fancy, just an overview. ArchivesCategories |
 RSS Feed
RSS Feed
